A discussion on Hair Growth and Diode Laser Hair Removal
Hair.
Hair is made of a tough protein called keratin, combined with a small amount of water and a binding agent to hold the keratin and water together. It is produced by a hair follicle. The human body has hundreds of thousands of hair follicles covering everywhere on the body except for the lips, the eyelids and the plantar aspect of the hand and foot (palms & soles). Each follicle produces many hairs throughout our lifetime.
Vellus hairs are short, fine, colourless hairs covering most of the body, except those areas covered with terminal hairs, which are coarse, pigmented hairs found on the scalp and eyebrows. They can transform into terminal hairs when stimulated by androgens (male sex hormones), especially those on the face, back, chest, abdomen, axillae, and genitalia at puberty, but they can also transform into terminal hairs with ageing. The number of hair follicles present in the skin is fixed at birth.
Although hair has a simple enough visual appearance, it is actually much more complicated than suggested by first impression and has a multitude of functions including:
- Transmitting sensory information
- Acting as a barrier to foreign particles.
- Regulating the temperature of our bodies by aiding the evaporation of perspiration.
- Assists in creating gender identity
And
- It is the only body structure that can completely renew itself without scarring.
To understand how laser can be utilised to reduce or remove hair from an area of the body, we first need to understand the structure of hair, how it is created and how it relates to neighbouring structures.
The Formation of Hair
Like skin, hair is a stratified squamous keratinized epithelium made of multi-layered flat cells whose rope-like filaments provide structure and strength to the hair shaft.
The hair forms part of a complex anatomical structure called the “Pilosebaceous Unit”.
The pilosebaceous unit is formed by an epidermal introflexion, or more accurately an invagination, in to the dermis, forming a pocket or sac which contains;
- the hair follicle
- the hair shaft
- the sebaceous gland; which makes sebum &
- the erector pili muscle (aka: arrector pili); which causes the hair to stand up when it contracts.
- In some areas of the body, an apocrine, sweat, gland will also be present.
Most simply, hair can be divided in to two main parts:
- The Hair Bulb or root - the part of the hair below the skin surface, which interacts with the other associated structures of the pilosebaceous unit as well as the dermis & hypodermis layers of the skin.
- The Hair Shaft - the visible part of the hair that protrudes out of the skin through a small hole called the “Follicular Ostium”.
The hair bulb forms the base of the hair follicle.
In the hair bulb, live hair cells are generated inside the follicle by the papilla. As the new cells divide and grow, the older cells lose their nucleus, die, and are compressed to form the keratin protein as they are forced along the follicle towards the scalp, building the hair shaft, which continues through the follicular ostium to form the visible hair. Blood vessels nourish the cells in the hair bulb, and deliver hormones that modify the growth and structure of the hair at different times of life.
Fig. 1. Diagram of a Hair Follicle
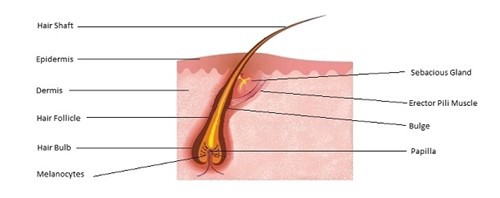
Structurally, the hair shaft is composed of an outer translucent cuticle and a central coloured cortex.
Hair colouring is created by pigment cells in the base of the hair follicle, producing melanin. There are two forms of melanin involved in hair colouring: Eumelanin gives brown or black colouring and pheomelanin gives yellow and red. With ageing, the pigment cells die and hair turns grey.
Hair Growth
Hair growth is not constant, but follows a cycle consisting of three phases:
Anagen
The active growth phase of hair follicles, during which the papilla cells in the root of the hair bulb are dividing rapidly and the follicle buries itself into the dermal layer of the skin to nourish the strand. The newly created cells grow, the older cells are compressed to form the Keratin protein, lose their nuclei and are forced along the follicle towards the scalp - pushing the old hair follicle out through the Follicular Ostium as they do so. During this phase the hair grows about 1 cm every 28 days.
During the early anagen stage, melanocyte stem cells (McSCs) located in the bulge region, migrate down the internal root sheath to the hair follicle matrix (where the actual strand of hair is formed). The McSCs then differentiate into pigment producing cells called melanocytes (the pigment produced by melanocytes is called “melanin” and it’s what gives your hair colour)
At any given time, most hair is growing and may stay in this active phase of growth for anything from several weeks to several years. At the end of the anagen phase, the follicle to go into the catagen phase.
Catagen
A short transition stage that occurs at the end of the anagen phase, signalling the end of the active growth of a hair. The first sign of catagen is the cessation of melanin production in the hair bulb and apoptosis (programmed cells death) of follicular melanocytes. This phase lasts for about 2–3 weeks while the hair converts to a club hair, when the part of the hair follicle in contact with the lower portion of the hair becomes attached to the hair shaft. This process cuts the hair off from its blood supply and from the cells that produce new hair. At the end of the catagen stage, the hair follicle enters the telogen phase.
Telogen
A resting phase which lasts several weeks to months, during which hair growth stops and the old hair detaches from the hair follicle. A new hair begins the growth phase, pushing the old hair out. When the body is subjected to extreme stress, as much as 70 percent of hair can prematurely enter a telogen phase. Thus hair begins to fall, causing a noticeable loss of hair. This condition is called telogen effluvium. The club hair is the final product of a hair follicle in the telogen stage, and is a dead, fully keratinized hair. Typically, fifty to a hundred club hair are shed daily from a normal scalp.
Fig 2. Diagram of the Stages of Hair Growth
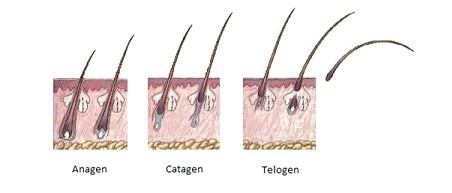
Obviously, not all hair is in the same phase at the same time, or else we would all periodically go completely bald as our hair fell out. Instead, all three phases occur simultaneously; one strand of hair may be in the anagen phase, while another is in the telogen phase.
In addition, the duration of the individual phases of hair growth vary from region to region around the body.
Table 1. Hair Growth - Average values
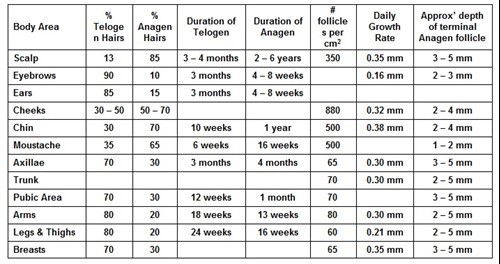
Factors affecting the growth of hair.
Several factors can interfere with the normal life cycle of hair. These include:
Age:
Generally, in both males and females, with the passing of time the renewal cycle slows down. In addition, the incidence of hair loss corresponds to chronological age. The older you get, the greater the chance of hair loss with slower growth of remaining hair
Blood Circulation:
The more blood reaching the hair bulb, the greater the delivery of oxygen and nutrients and the better the growth rate.
Vitamins & Minerals:
Vitamins B5 and B6, along with Vitamins A, E & C, have a beneficial effect on hair growth. Adequate levels of Iron, Zinc, Iodine and Silica are also important
Climate:
Increased ambient temperature leads to vasodilation, increasing the blood supply to the dermal layer and leading to the improved growth rate described above. On the other hand, the sun can damage the scalp and hair.
Diet:
Rate of growth of hair is dependent on health of the scalp and the follicles, which is improved by a diet rich in fresh fruit and vegetables to provide good nutrition.
Exercise:
Exercise leads to improvement in general health as well as increasing blood supply to the dermis, which provides improved oxygenation and nutrient distribution, all of which are conducive with an elevated growth rate.
Stress:
Increased stress is one of the most common causes of sudden hair loss. The hormones associated with increased stress levels can put an increased number of follicles into the telogen (resting) phase of the hair cycle - a condition known clinically as telogen effluvium.
Genetics:
Beyond our individual control; genetic factors are responsible not just for hair colour, but also hair density, texture and growth. In those genetically prone to hair loss; dihydrotestosterone (DHT) initiates miniaturisation of the hair follicles.
Hormones:
Androgen Hormones (male hormones), produced by the testes and in smaller quantities by the adrenal glands, have a direct action on hair growth.
In females, an increased production of these same androgen hormones causes growth in uncommon areas. Meanwhile, the female oestrogen hormone inhibits hair production by blocking or delaying the regrowth of hair.
Both hyper- and hypo- thyroidism can lead to alopecia, however it tends to only happen in severe and prolonged conditions rather than mild (sub-clinical) conditions. As a result of the long hair cycle, hair loss due to thyroid disease becomes apparent several months after the onset of thyroid disease. In such cases, paradoxically the hair loss may follow the treatment for the thyroid and the thyroid medication may be erroneously blamed, leading to withdrawal of treatment, which in turn may worsen the hair loss.
Epidermal conditions:
A number of such conditions can contribute to slower hair growth, including:
- Ringworm infections
- Folliculitis
- Psoriasis
- Seborrheic dermatitis
Anomalies in the growth of hair
Below are details of some of the more common anomalies you may come across:
Hypertrichosis:
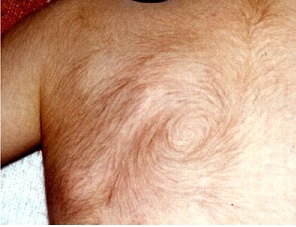
This is the medical term for excessive hair growth that affects any gender.
Hypertrichosis (also called Ambras syndrome) is an abnormal amount of hair growth over the body; extensive cases of hypertrichosis have informally been called werewolf syndrome, because the appearance is similar to the mythical werewolf.
The two distinct types of hypertrichosis are generalized hypertrichosis, which occurs over the entire body, and localized hypertrichosis, which is restricted to a certain area.
Hypertrichosis can be either congenital (present at birth) or acquired later in life. The excess growth of hair occurs in areas normally subject to very light and thin hair such as:
- Lips
- Areola
- Eyebrow
- Umbilicus
- sternum
Can be the result of a variety of causes including:
- hormonal factors (increase of androgens),
- pharmacological hormonal factors (antidepressants, diuretics, corticosteroids),
- metabolic factors (heavy diet),
- psychogenic factors (anorexia, bulimia, stress).
Hirsutism
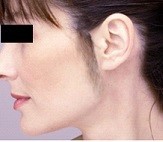
Hirsutism is classically seen as the excessive hairiness on women in those parts of the body where terminal hair is normally absent or minimal, such as a face, shoulders, abdomen or chest. It refers to a male pattern of body hair (androgenic hair) and is thus primarily of cosmetic and psychological concern.
Hirsutism is a medical sign rather than a disease but may be an indication of a more serious medical condition, especially if it develops well after puberty.
Hirsutism can be caused by either an increased level of androgens, the male hormones, or an over sensitivity of hair follicles to those androgens.
A range of conditions may increase a woman's normally low level of male hormones, including:
- Poly-cystic ovary syndrome (PCOS), by far the most common cause currently
- Congenital adrenal hyperplasia, mostly caused by 21-α hydroxylase deficiency
- Cushing's disease
- Excessive Growth hormone (acromegaly)
- Ovarian Tumours
- Adrenal gland cancer,
- Von Hippel–Lindau disease
- Insulin resistance
- Stromal hyperthecosis (SH) - in postmenopausal women
- Obesity: Results in a peripheral conversion of androgens to oestrogen, which is the same mechanism as occurs in polycystic ovary syndrome, PCOS.
- Use of certain medications such as tetrahydrogestrinone, phenytoin & minoxidil.
- Porphyria cutanea tarda
The amount and location of the hair is measured by a Ferriman-Gallwey score.
Keratosis Pilaris:
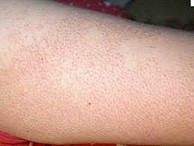
Also known as: follicular keratosis, lichen pilaris, or more colloquially as "chicken skin", Keratosis Pilaris is a common autosomal-dominant genetic follicular condition characterised by the appearance of rough, slightly red bumps on light skin and brown bumps on darker skin.
It most often appears on the back, outer sides of the upper arm (sometimes extending on to the forearm), face, thigh, and buttocks; but Keratosis Pilaris can also occur anywhere on the body except on glabrous skin (such as the palms of the hands or soles of feet). When the lesions appear on the face, they may be mistaken for acne.
Keratosis Pilaris is a condition characterised by excessive production of keratin. The excess keratin, surrounds and entraps the hair follicles in the pore. This causes the formation of hard plugs - a process known as “hyperkeratinisation”. Many Keratosis Pilaris bumps contain an ingrown hair that has coiled as a result of the keratinized skin's "capping off" the hair follicle, preventing the hair from exiting. The hair grows encapsulated inside the follicle.
Ingrown hair:
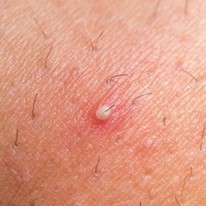
A condition where hair curls back, or grows sideways, into the skin.
The condition is most prevalent among people who have coarse or curly hair. It may or may not be accompanied by an infection of the hair follicle (folliculitis) or "razor bumps" (pseudofolliculitis barbae), which vary in size.
While ingrown hair most commonly appears in areas where the skin is shaved or waxed (beard, legs, pubic region), it can appear anywhere.
Anything which causes the hair to be broken off unevenly with a sharp tip can cause ingrown hairs. Shaving is the leading cause, followed by waxing and tight clothing.
Folliculitis:
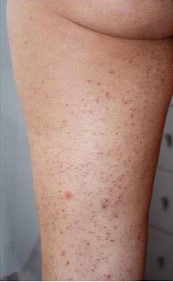
The infection and inflammation of one or more hair follicles.
The condition may occur anywhere on the skin with the exception of the palms of the hands and soles of the feet, but is typically found on the face, chest, back, arms, legs, and head.
The resulting rash may appear as pimples that come to white tips.
Folliculitis starts with the introduction of a skin pathogen to a hair follicle, often following damage to the follicle.
Hair follicles can also be damaged by friction from clothing, an insect bite, blockage of the follicle and shaving. The damaged follicles are then infected with the bacterium Staphylococcus or Pseudomonas aeruginosa.
